Featured Aesthetics
Microneedling – Advanced Collagen Boost with VAMP, PRP, PRF &/or Exosomes
Microneedling
Microneedling in Orange County
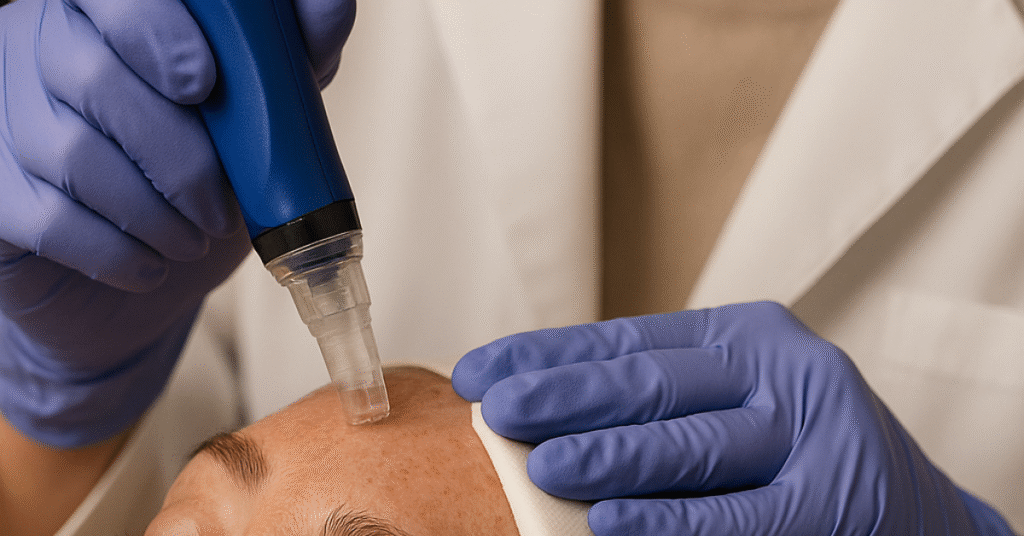
Lift, smooth, and revive your skin with the latest in collagen induction therapy.
At our clinic, we combine FDA-cleared SkinPen® microneedling with powerful biologic enhancements like VAMP (salmon DNA therapy), PRP, PRF, and exosomes to deliver transformative skin rejuvenation. Whether you want a subtle refresh or a dramatic glow-up, we’ll tailor your treatment to your skin’s needs.
What is Microneedling?
Microneedling, also known as collagen induction therapy, uses ultrafine needles to create controlled micro-injuries in the skin. This triggers your body’s natural healing response, stimulating the production of collagen and elastin — essential proteins that keep skin smooth, firm, and youthful.
The SkinPen® difference:
- FDA-cleared and medical-grade
- Safe for all skin types
- Adjustable needle depth for customized results
- Proven to improve skin texture, tone, and firmness
Why Choose SkinPen® with Biologic Boosters?
While microneedling alone delivers amazing results, pairing it with biologic enhancements can accelerate healing, maximize collagen production, and enhance skin regeneration. We offer four powerful add-ons:
VAMP – Salmon DNA Therapy
VAMP (short for Vitality and Anti-aging Marine Peptides) harnesses purified salmon DNA, which closely resembles human DNA, to deeply hydrate, repair, and rejuvenate the skin.
Benefits:
- Improves elasticity and firmness
- Boosts skin hydration at a cellular level
- Enhances glow and radiance
PRP – Platelet-Rich Plasma
PRP uses a small sample of your own blood, spun to concentrate growth factors, which are then applied during or after microneedling.
Benefits:
- Speeds recovery
- Stimulates collagen production
- Improves skin texture and tone
PRF – Platelet-Rich Fibrin
The next generation of PRP, PRF is spun at a slower speed, preserving more white blood cells and stem cells for greater regenerative potential.
Benefits:
- Higher concentration of platelets (up to 10x your body’s baseline)
- Slower release of growth factors for prolonged rejuvenation
- 100% natural — no anticoagulants added
Exosomes
Derived from stem cells, exosomes act as cell-to-cell messengers, delivering powerful growth signals to repair and regenerate tissue.
Benefits:
- Supports faster healing
- Reduces inflammation
- Boosts collagen and elastin synthesis
Treatment
Microneedling is a non-surgical, minimally invasive skin rejuvenation technique that does require a local anesthetic to make the treatment comfortable. The clinician will use a pen-like device or a device that has a handheld component with built-in needles that may or may not include radiofrequency. The clinician controls the depth of needle penetration from 0.1mm-3.5mm depending on the area being treated or your skin condition. The treatment can be safely performed on delicate areas of the face like upper and lower eyelids, the upper lip, and the cheeks. The treatment time is about 45 min. There is minimal downtime associated with this treatment but it is expected to have some redness for the first 24 hours and you may sensitivity for about 72 hours.
Microneedling Benefits:
- Stimulating collagen production
- Reduction in fine lines and wrinkles
- Reduction in the appearance of acne scars
- Reduction in the appearance of stretch marks
- Improving skin elasticity or tightening the skin
- Balancing out uneven skin tone
- Reducing the appearance of sunspots or age spots and other damage caused due to environmental exposure
- Reduction in the pore size
Microneedling Pre & Post Care Instructions
Pre-Treatment Instructions
- Do not wear makeup on the day of treatment.
- Medications or supplements that may increase your risk of bleeding should be avoided 3-7 days before treatment. These include, but are not limited to, anticoagulant medication, antiplatelet medication, aspirin, aspirin-containing medications, non-steroidal anti-inflammatory drugs, fish oil, flaxseed, garlic, ginkgo biloba, ginseng, omega 3 fatty acids, St. John’s Wort, and vitamin A or E. You should consult with your physician before discontinuing anything prescribed or recommended by your physician.
- Avoid antihistamines and anti-inflammatory drugs 1 week prior to treatment. These negate the effects of the procedure. The body’s histamine and inflammatory responses are needed post-treatment.
- Excess hair may need to be shaved. Men should be clean shaved.
- Avoid sun exposure and tanning beds for 4 weeks prior to treatment and use a sunscreen of at least SPF 30 daily to ensure coverage against UVA and UVB rays.
- Avoid self-tanners 4 weeks prior to treatment.
- Consult with your physician if you have been on photosensitizing medication within the last 12 months.
- Avoid chemical peels and laser treatments in the area to be treated for 4 weeks prior to your treatment.
- Avoid skin irritants (products containing hydroxy acids, hydroquinone, retinoids, vitamin C, etc.) 3 days prior to your treatment.
- Avoid waxing, tweezing, and use of chemical depilatories 1-2 weeks prior to treatment.
- If you have a history of cold sores of Herpes Simplex Virus, you may be recommended to take an antiviral medication before treatment.
- Avoid neuromodulators and/or dermal fillers 2 weeks before your treatment.
- Notify the office staff if you develop a cold sore, acne, open lesions in the area being treated, or experience any type of illness prior to your treatment.
Post-Treatment Instructions
- The initial 72 hours post-procedure are the most critical.
- Avoid direct sun and heat. This includes simple day-to-day tasks such as gardening, cooking over a hot stove for a long period of time, sitting next to a bonfire or fireplace, etc.
- Discontinue the use of any Alpha-Hydroxy products. You may resume your home care regimen when the skin is no longer flaking and peeling.
- Use hydrating and reparative products. Products rich in soothing and healing ingredients are best to encourage new, healthy cell growth. Peptides, antioxidants, stem cells, Vitamin A, C, and E, and growth factors work very well.
- Use physical sunscreen. Suncare products should be applied no less than every 30-90 minutes. Do not go outside without sun protection (even on a cloudy day).
- Minor peeling and flakiness will occur after a few days. Don’t pick at the loose skin.
- Limit exercise the first week.
- Drink plenty of water.
- Call our office if you experience excessive redness, swelling, pain, or drainage as they might indicate an infection.
